
Percutaneous Autograft Delivery Technology
The Avitus® ArchiMIS™
The Avitus® ArchiMIS™ – is an industry first for percutaneous autograft delivery.
Indications For Use
The Avitus® ArchiMIS™ is intended:
- To be used for the delivery of autograft or hydrated allograft bone graft material to an orthopaedic surgical site.
A percutaneous controlled delivery experience for
autologous gold-standard bone grafting
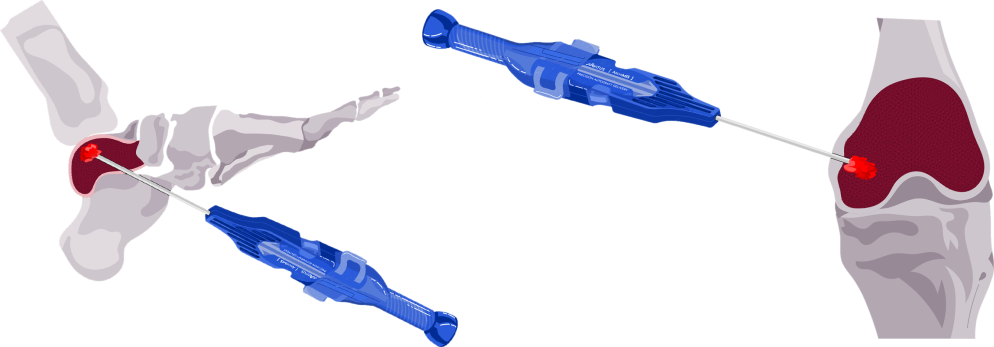
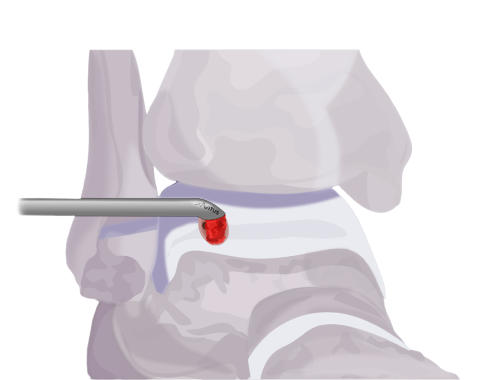
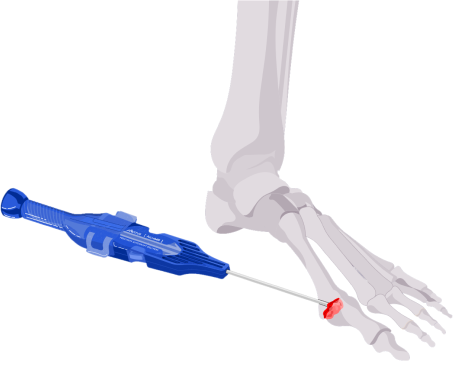
Deliver the gold-standard with versatility
The ArchiMIS™ includes two delivery cannula options:
4.0 mm (OD) Angled Delivery Cannula: for applications such as Talar Dome OCD
3.8 mm (OD) Straight Delivery Cannula: for applications such as MIS Fusions, Cysts, etc.
ArchiMIS™ - Video Reel
Dr. San Giovanni │ Large OCD Repair
With Proximal Tibia Autograft
Dr. Pereira │ Patella Cyst Grafting
With Distal Femur Autograft
Dr. San Giovanni │ Retrograde Technique
Cadaveric Demostration
Dr. Scott C. Carrington | TIBIAL PLAFOND OCD
WITH CYST With Proximal Tibia Autograft
Dr.Bradley Abicht | MIS MPJ FUSION
How to Use ArchiMIS
Dr Abicht – ArchiMIS – TN Fusion Calc Harvest
ArchiMIS – Percutaneous TN Fusion with Calc Harvest

Testimonials


A percutaneous autograft delivery experience
An industry first for autograft. Unlock the gold-standard bone graft for MIS.
Request ArchiMIS!
- 2017. Minas et al (paley institute). 24 patients received “Sandwich” technique of autologous bone graft fill of an Knee OCD with an ACI (autologous chondrocyte implant on top of the cancellous bone graft) for OCD treatment. ACI full standwich technique provided excellent and superior survival rates (87% at 5 and 10 years) with significant improvements in pain and function over midterm to long term follow up. Patient satisfaction rate was 96%. This is a technique for joint preservation. https://sci-hub.ru/10.1177/0363546517738000
- 2014. Steven Raikin MD. Describes technique for Tibial Plafond OCDs utilizing autologous bone graft for cystic OCDs. https://sci-hub.ru/10.1007/978-3-642-45097-6_9
- 2019. Nikolopoulos et al. 41 patient study. 2 year follow up. Proximal Tibia Autograft with Periosteal flap cover used to repair large osteochondral lesions of the talar dome (OCL). No donor site complications. Average VAS of OCD went from 7.7 to 1.1 1 year after surgery and 0.4 at 2 years or more after surgery. Patients AOFAS scores ranged from 85 to 100 1 year and 2 year poster operatively with a mean of 95.0. 80.5% of patients reported excellent results and 19.5% reported good results based on AOFAS and FADI scores. 85.4% of patients reported being able to perform activity at the same level as prior to the onset of their symptoms. 14.6% reported being able to perform a lower level of physical activity compared to before the onset of their symptoms. This paper features a medial malleolar osteotomy (which is more invasive than ArchiMISTM approach; the ArchiMISTM enables this procedure to be performed without a medial malleolar osteotomy (potential to reduce morbidity). https://journals.sagepub.com/doi/10.1177/2473011419874039
- 2006. Zengerink, Ferkel et al. Cites the use of proximal tibia cancellous bone graft for large OCD defects in conjunction with debridement of subchondral bone. https://sci-hub.ru/10.1016/j.fcl.2006.03.008
- 2007. Basad et al. MACI Method in conjunction with Autogenous Cancellous bone graft. 12 patients with 2 year follow up. Deep debridement of sclerotic subchondral bone was performed, followed by press-fit filling of the defect with autogenous cancellous bone. In a follow on 2nd operation, a double layer of MACI was fixed within the defect with fibrin glue. 6 month MRI showed subchondral edema within the bone graft disappeared. Within a year, MRI signal intensity of the cartilage repair approximated to that of the healthy surrounding cartilage. Thickness of cartilage increased from 1mm to 1.8mm. https://pubmed.ncbi.nlm.nih.gov/18180588/
- 2022. Holwein et al. MRI follow ups 2+ years post operatively in 21 patients with Knee OCLs. Patients received Distal Femur Autologous Cancellous Bone or Iliac Crest cancellous bone graft in conjunction with a MACT (Matrix cap for cartilage layer). Weightbearing restricted for 6 weeks. Cancellous bone graft was used to optimize the shaping of the defect. The combination of autologous cancellous bone graft with MACT contribute to significantly improve patients’ activity levels post operatively. https://journals.sagepub.com/doi/full/10.1177/19476035221102571
- 2018. Sawa et al. 12 patient study. Distal Tibia autogenous cancellous graft was used with cartilage fragment fixed with suture on top. This paper also features a medial malleolar osteotomy (7 out of 12 patients requested to remove the medial malleolar osteotomy screw at 1.5-2 years post op although non symptomatic). If injecting autologous bone through ArchiMIS, the medial malleolar osteotomy screw would not be needed (saves cost and potential reduction in morbidity). At one year MRI, no scans showed any signs of osteochondral graft instability. The chondral fragment showed a smooth surface on 2nd look arthroscopy. 100% patient satisfaction with a range of AOFAS ankle-hindfoot outcome scores of 90-100. https://journals.sagepub.com/doi/10.1177/2473011418S00106
- 2015. 17 patient study. 1/16 cases was performed without a medial malleolar osteotomy. 15/16 cases were done with a medial malleolar osteotomy. Defective cartilage and necrotic subchondral bone was debrided, sclerotic bone zones were microfractured, autologous cancellous bone harvested from the proximal tibia and impacted into the prepared bony defect to restore the outline of the talar shoulder. Then porcine collagen membrane was placed onto the cancellous bone and fixed with fibrin glue. Partial weight bearing for 6 weeks after surgery.
- 2004. Takao et al. 39 patient study. Study shows the treatment of osteochondral lesions of talar benefits from removing the degenerative cartilage. https://pubmed.ncbi.nlm.nih.gov/14977656/
- 2016. Haskell et al. 22 patients (23 ankles). Cancellous autograft bone plug from distal tibia implanted into a drilled out talar lesion through a small arthrotomy (small incision). Distal Tibia Bone Grafting is a safe and effective treatment for large talar OCLs. Results were comparable to reported literature describing OCL treatment techniques. 23 month follow up. No re-operations. AOFAS hindfoot mean scores improved from 67 (51-83 range pre-op) to 88 (76-100 post-op). https://journals.sagepub.com/doi/10.1177/2473011416S00161
- 2012. Anders et al. 41 patients. Retrograde drilling with cancellous autograft for subchondral cysts with intact cartilage. Results indicate that autologous cancellous bone grafting is an efficient option for retrograde approach where OCL of talus with intact cartilage surface after failed conservative treatment. Subchondral bone is resected and autologous bone graft provides extended revitalization for OCL healing. https://sci-hub.ru/10.1007/s00264-012-1530-9
- 2021. Alisi et al. 16 patients. Retrospective analysis. Treatment of benign bone cysts (SBC/ABC) with minimally invasive percutaneous curettage and a local autologous cancellous bone graft is a simple and effective modality with a promising outcome in the local control of recurrence and in enhancing bony consolidation. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8889432/pdf/ABJS-10-104.pdf
- 2021. Hu et al. 18 patients. Case series. Iliac crest cancellous bone graft packed into OCDs with periosteal flap transfer through a medial malleolar osteotomy. 24 month follow up. The main reason for the osteotomy is to put graft into the OCD (ArchiMIS prevents that). Procedure provided early rehabilitation for patients. 12 of 18 patients elected to have their medial malleolar hardware removed at 12.2 (mean) weeks post op. All patients were able to return to recreational sports or at least moderately heavy labor. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8237210/
- 2022. Zhang et al. 23 patients. At least 22 month follow up. 21 of 23 patients returned to sport at their previous level. 2 returned at a lower level compared with preinjury. 1/23 complications due to medial malleolar osteotomy. Debridement of OCL + using autologous OATs as graft. https://bmcmusculoskeletdisord.biomedcentral.com/articles/10.1186/s12891-022-05043-z
- 2015. Usuelli et al. Describes surgical technique of utilizing cancellous bone harvested from calcaneus to rebuild bony anatomy to the surface of the cartilage in preparation for a cartilage graft to be laid on top and then sealed with fibrin glue. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4523902/
- 2023. Yokoe et al. Surgical technique for iliac crest bone plug in conjunction with retrograde cancellous bone grafting with intact cartilage. https://www.mdpi.com/2077-0383/12/10/3431
- 2017. Kanatli et al. Utilized cancellous autologous bone from iliac crest to fill cystic OCDs after debriding and microfracturing the prepared defect. https://www.sciencedirect.com/science/article/pii/S2212628717302116#:~:text=Unhealthy%20cartilage%20and% 20subchondral%20bone,closest%20portal%20to%20the%20lesion.
General references for ArchiMIS / the use of autologous bone in OCD applications

